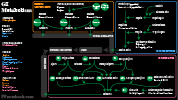
II. Physiology: Gastrointestinal Motility
- Chewing (mastication)
- Chewing breaks apart food for greater surface area, allowing for later processing and absorption
- Nerve control: CN 5 (Trigeminal Nerve)
- Muscles of Mastication
-
Swallowing
- See Swallowing
- See Dysphagia
- Oropharyngeal Stage
- Esophageal Stage
- Peristalsis
- See Ileus
- See Constipation
- See Diarrhea
- Peristalsis propels food from the Stomach forward through the intestinal tract
- Timing
- Solid Food exits the Stomach after 1-3 hours
- Food exits the Small Intestine (at the ileocecal valve) after 4-6 hours
- Food exits the colon with Defecation typically after 1-2 days
- Nerve Control: CN 10 (Vagal Nerve)
- Stimulates peristalsis
- Myenteric Plexus (Auerbach's plexus) between the bowel's circular and longitudinal Muscles
- Examples of dysfunction: Achalasia, Hirschsprung's Disease
- Relaxes sphincters
- Promotes glandular secretion
- Meissner's Plexus in the submucosal layer
- Stimulates peristalsis
III. Physiology: Energy Sources
- Background
- Ingested food is lysed into small component molecules for intestinal absorption
- Starches and Disaccharides are lysed into Monosaccharides
- Proteins are lysed into Amino Acids and some short-chain peptides
- Fats are lysed into free Fatty Acids and Cholesterol
- Intestinal epithelial cell absorption
- Simple diffusion (passive absorption) of free Fatty Acids, monoglycerides and water
- Active transport (esp. Sodium-Potassium ATPase pump) for most other molecules
- Portal circulation carries most absorbed energy sources to liver (except fats)
- Carbohydrates (the Monosaccharides Glucose, fructose and galactose)
- Proteins (Amino Acids and short-chain peptides)
- Short fatty-acids (remainder of fats are carried by Lymphatics)
- Lymphatics carry most absorbed fats
- Fats are carried by Chylomicrons via Lymphatics after intestinal absorption (see below)
- Malabsorption has many mechanisms
- Lactose Intolerance (Lactase Deficiency)
- Pernicious Anemia (Vitamin B12 Deficiency from Intrinsic Factor deficiency)
- Celiac Disease (gluten-mediated injury to intestinal villi)
- Ingested food is lysed into small component molecules for intestinal absorption
-
Carbohydrates (4 kcals/g)
- See Carbohydrate Metabolism


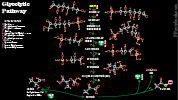

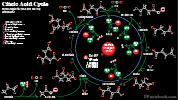
- Stores exhausted in first day of starvation
- Starches and Disaccharides are cleaved into Monosaccharides before intestinal absorption
- Mediated by Stomach acid and Salivary, intestinal and Pancreatic Enzymes (see below)
- Starches (Glucose polymers, cleaved by amylase into maltose)
- Glycogen
- Amylose
- Disaccharides
- Monosaccharides
- Glucose
- Fructose
- Galactose
-
Protein (4 kcals/g)
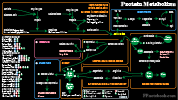
- Last to be catabolized in starvation
- Proteins are broken down to Amino Acids and some small peptides before absorption
- Mediated by Stomach acid, pepsin, trypsin and peptidases (see below)
- Proteins (polypeptides)
- Long chains of peptides (which in turn are chains of Amino Acids)
- Peptides
- Short chains of Amino Acids (two or more)
- Amino Acids
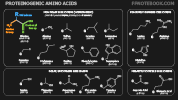
- Twenty common, Proteinogenic, Amino Acids occur in humans, in which 9 are essential (must be ingested)
- Fat (9 kcals/g)
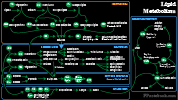
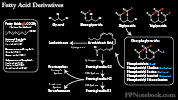
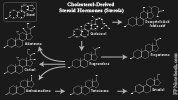
- Long term energy source
- Intestinal Digestion and Absorption of fats
- Duodenal bile salts emulsify fats into small droplets
- Enzymatic breakdown by intestinal and pancreatic agents
- Lipase (intestinal, pancreatic) lyse Triglycerides to monoglycerides and free Fatty Acids
- Esterases lyse Cholesterol to free Cholesterol and free Fatty Acids
- Phospholipases lyse phospholipids to free Fatty Acids and lysophospholipids
- Small micelles form from fat breakdown products and bile acids
- Micelles carry fats to intestinal epithelial cell brush border for absorption
- Bile salts allow for absorption of polar lipids
- Bile salts are reclaimed by enterohepatic circulation
- Bile salts absorbed in ileum are transported back to liver via portal circulation
- Intestinal Epithelial cell Processing of Fats
- Re-forming of lipids
- Triglycerides re-form from free Fatty Acids and monoglycerides
- Cholesterol esters re-form from free Fatty Acids and Cholesterol
- Phospholipids re-form from free Fatty Acids and lysophospholipids
- Chylomicrons
- Form from Apoproteins combined with Triglycerides, Cholesterol to phospholipids
- Chylomicrons move from intestinal epithelial cells into Lymphatic System
- Triglycerides are carried by Chylomicrons to Muscle and fat cells
- Triglycerides are lysed into free Fatty Acids by capillary LipoproteinLipase
- Free Fatty Acids are then absorbed by Muscle and fat cells
- Triglycerides reform from free Fatty Acids within Muscle and fat cells (esterification)
- Other Lipoproteins (VLDL, LDL, HDL)
- Form from Cholesterol processing in the liver
- Re-forming of lipids
IV. Physiology: Digestion Mediators
- Images
- Background
- Some promoters of Digestion at one level inhibit Digestion proximally
- Cholecystokinin promotes Pancreatic Enzyme and Gall Bladder function, while inhibiting gastric motility
- Secretin promotes hepatic bile acid secretion, but decreases Gastrin secretion (and gastric and intestinal function)
- Local neurologic negative feedback loops also modify intestinal function
- Small Bowel distention decreases gastric motility and delays gastric emptying
- Digestion Mechanisms
- Hydrolysis
- Addition of water in process of cleaving complex Carbohydrates, Proteins and fats
- Hydrolysis
- Gastrointestinal mucosa is protected from acidity (bicarbonate secretion) and digestive enzymes (mucous secretion)
- Protective factors decreased by NSAIDs and Aspirin, emotional stress, Helicobacter Pylori
- Examples of dysfunction: Cystic Fibrosis, Peptic Ulcer Disease
- Some promoters of Digestion at one level inhibit Digestion proximally
- Mouth
- Salivary Amylase
- Breaks down starches (to maltose and other sugars)
- Salivary Amylase
-
Stomach
- Background
- Pepsinogen
- Hydrochloric Acid (HCL)
- Breaks down starches
- Aids in mineral absorption and bacterocidal activity
- Released by parietal cells
- Triggered by Vagus Nerve, Gastrin, Histamine and Proteins within the Stomach
- Intrinsic Factor
- Glycoprotein released by parietal cells
- Intrinsic Factor deficiency occurs in Pernicious Anemia (Vitamin B12 Deficiency)
- Facilitates Vitamin B12 absorption from Small Intestine
- Triggered by Stomach and duodenal distention
- Suppressed by low gastric pH and intestinal fat
-
Gastrin
- Stimulates HCl acid secretion by parietal cells and enzyme secretion from Pancreas
- Also increases peristalsis and relaxes pyloric sphincter and ileocecal valve
- Released from Gastrin cells in Stomach antrum
- Stimulated by Vagus Nerve, duodenal distention and Proteins within the Stomach
- Suppressed by Secretin, gastric inhibitory polypeptide and decreased Stomach pH
- Abnormally increased in Zollinger Ellison Syndrome (gastrin Secreting tumor)
-
Small Intestine
- Background
- Intestinal mucosa is protected by an alkaline mucus (from Brunner's Glands)
- Epithelial cells in Crypts of Lieberkuhn (within intestinal villi)
- Release most intestinal digestive enzymes (aside from Pancreatic Enzymes)
- Stimulated by Vagus Nerve and direct contact with food
- Carbohydrate Digestion
- Protein Digestion
- Peptidases
- Cleaves peptides into Amino Acids
- Enterokinase
- Activates trypsinogen to trypsin
- Activates chymotrypsinogen to chymotrypsin
- Activates procarboxypolypetidase to carboxypolypetidase
- Peptidases
- Fat and Cholesterol Digestion
- Intestinal Lipase
- Metabolizes lipids to Glycerol and Fatty Acids
- Intestinal esterases
- Metabolize Cholesterol esters to free Cholesterol and Fatty Acids
- Intestinal Lipase
- Other enzymes
- Secretin
- Polypeptide (27 Amino Acids) secreted from duodenal and jejunal mucosa
- Functions
- Decreases Gastrin secretion, and gastric acid secretion
- Decreases intestinal motility
- Promotes Stomach pepsin release
- Promotes bile acid secretion from liver
- Promotes bicarbonate secretion (and water) from Pancreas
- Lowers Serum Glucose
- Factors that increase Secretin levels
- Vagal Nerve Stimulation
- Food, fat or acid within the Small Intestine
- Gastric inhibitory peptide (GIP)
- Decreases Gastrin secretion
- Decreases gastric emptying
- Cholecystokinin
- Polypeptide (33 Amino Acid) secreyted from the upper small intestinal mucosa
- Functions
- Decreases gastric motility
- Promotes Pancreatic Enzyme and bicarbonate secretion
- Promotes Gall Bladder contraction and sphincter of oddi relaxation (intestinal bile acid secretion)
- Vasodilates intestinal mucosa vessels
- May also mediate satiety
- Factors that increase Cholecystokinin levels
- Fatty Acids in the duodenum (some Amino Acids can also stimulate release)
- Vagal Nerve Stimulation
- Bulbogastrone
- Suppresses acid secretion from gastric parietal cells
- Secretin
- Background
-
Pancreas
- Background
- Bicarbonate secreted by pancreatic ductule cells neutralizes Stomach acid in the duodenum
- In Pancreatitis, exocrine enzymes are activated while still within the Pancreas, resulting in inflammation
- Exocrine Cell Secreted Enzymes (vagal stimulated, as well as by cholecystokynin and Secretin)
- Amylase
- Breaks down starch to Oligosaccharides and ultimately sugars (e.g. Glucose, maltose)
- Trypsinogen
- Enterokinase (enteropeptidase) activated to trypsin
- Trypsin cleaves Proteins into peptides and Amino Acids
- Trypsin also activates Chymotrypsinogen and Procarboxypolypeptidase
- Chymotrypsinogen
- Trypsin activated to chymotrypsin
- Chymotrypsin is a protease (cleaves Proteins into peptides and Amino Acids)
- Procarboxypolypeptidase
- Trypsin activated to carboxypolypeptidase
- Carboxypolypeptidase is a protease that cleaves Proteins at their C-Terminal end
- Lipase (pancreatic Lipase, steapsin)
- Hydrolyzes Triglycerides into Fatty Acids and monoglycerides
- Cholesterol esterase
- Breaks down Cholesterol ester into free Cholesterol and Fatty Acids
- Phospholipase
- Hydrolyzes phospholipids into Fatty Acids
- Nuclease (nucleodepolymerase, polynucleotidase)
- Cleaves DNA and RNA Nucleic Acids into Nucleotides
- Amylase
- Endocrine Enzymes
- Insulin
- Secreted by pancreatic beta islet cells
- Promotes liver, fat and Muscle Cell update of Blood Glucose
- Increases Triglyceride synthesis, and glycogen synthesis (when Glucose levels are high)
- Increases intestinal motility
- Glucagon
- Secreted by pancreatic alpha islet cells in response to low Blood Glucose levels
- Stimulates glycogenolysis and Gluconeogenesis, increasing Blood Glucose concentration
- Stimulates lipolysis, increasing blood Fatty Acid concentration
- Decreases intestinal motility
- Somatostatin
- Secreted by pancreatic delta islet cells
- Triggered by increased Blood Glucose and Amino Acid concentrations
- Also secreted by the Hypothalamus with CNS effects (decreased GH, TSH, Prolactin)
- Inhibits Insulin and Glucagon secretion, as well as pancreatic exocrine enzyme secretion
- Decreases gastric acid secretion by direct action at parietal cells
- Decreases gastric emptying and peristalsis
- Secreted by pancreatic delta islet cells
- Insulin
- Background
-
Liver (Hepatocytes)
- Bile Acids and Salts
- Bile acids surround ingested lipids (forming micelles) and aid in lipid intestinal aborption
- Bile acid emulsified fats are also more easily catalyzed by Lipase
- Micelles transport lipids to intestinal villi for absorption
- Primary bile acids are derivatives of Cholic acid and Chenodeoxycholic Acid
- Produced via CYP450 mediated Cholesterol metabolism
- Circulate through the intestinal tract and reabsorbed and reclaimed
- A smaller amount (600 mg) of bile acids are lost in stool and sythesized each day in the liver
- Bile acids surround ingested lipids (forming micelles) and aid in lipid intestinal aborption
- Bile Pigment
- Bilirubin and Biliverdin are breakdown products of Hemoglobin
- Bilirubin is conjugated in the liver and excreted into common bile duct in bile
- Fat-Soluble Vitamin Storage and Metabolism
- Drug Metabolism and Detoxification
- Cytochrome P450 mediated Drug Metabolism (oxidation, reduction and hydrolysis)
- Drug conjugation for excretion
- Bile Acids and Salts
- Gallbladder
- Stores bile produced in the liver
- Gall Bladder contraction and release of bile acids into duodenum on ingestion of lipids
- Stimulated by Cholecystokinin
- Inhibited by vagal nerve
-
Large Bowel
- Mucous and epithelial cells secrete mucus and bicarbonate
- Activity
- Lubricates and protects the colon lining
- Solidifies stool
- Neutralizes Bacterial Toxins
- Control
- Triggered by direct food contact
- Triggered by vagal nerve stimulation
- Suppressed by Sympathetic System
- Activity
- Mucous and epithelial cells secrete mucus and bicarbonate
V. Physiology: Appetite Modifiers
- Leptin
- Protein secreted from adipose tissue (Protein increases relative to adipose amount)
- Triggers Hypothalamus to suppress feeding
- Peptide YY (PYY)
- Peptide released from ileum and colon to decrease appetite
- Increases after meals, and decreases while Fasting
- Ghrelin
VI. Anatomy: Images
-
 Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
-
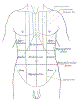 Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
-
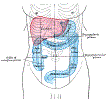 Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
-
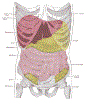 Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
-
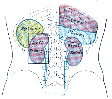 Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
-
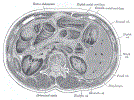 Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
-
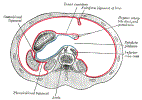 Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
-
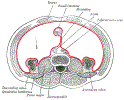 Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
Lewis (1918) Gray's Anatomy 20th ed (in public domain at Yahoo or BartleBy)
VII. References
- Goldberg (2014) Clinical Physiology, Medmasters, Miami, p. 120-31
- Kalra, Yetiskul, Wehrle, Tuma. (2021) Liver physiology, StatPearls, accessed 1/7/2022 online