II. Definitions
-
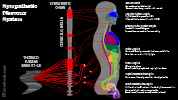
Sympathetic Nervous System
- Part of Autonomic Nervous System with activity that typically counters the Parasympathetic Nervous System
- Energy expending (catabolic) system, activated in stressful situations (e.g. emergency fight or flight)
- Contrast with the Parasympathetic Nervous System, an energy conserving system activated at times of rest
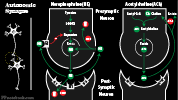
- Catecholamines
- Catecholamines act as Sympathetic System neuromodulators, binding adrenergic and Dopaminergic Receptors
- Catecholamines contain a catechol (benzene ring with 2 hydroxyl groups) derived from the Amino AcidTyrosine
- Endogenous Catecholamines are synthesized in the Adrenal Gland and postganglionic sympathetic Neurons
- Catecholamines include Epinephrine, Norepinephrine and Dopamine
- Sympathomimetics (Adrenergic Agonist)
- Sympathomimetics are agents that mimic the activity of postganglionic sympathetic Neurons
- Sympathomimetics include exogenous Catecholamines, as well as other agents with sympathetic activity
- Direct Sympathomimetics bind specific Adrenergic Receptors (a1, a2, b1, b2, d1-5) to trigger sympathetic activity
- Indirect Sympathomimetics enter the presynaptic Neuron and displace Norepinephrine from their storage Vesicles
- Mixed Sympathomimetics act both indirectly (Norepinephrine displacement) AND directly (Adrenergic Receptor binding)
IV. Physiology: Receptor Types
-
Alpha Adrenergic Receptor
- Alpha 1 Adrenergic Agonists Vasoconstrict, increase myocardial contractility, decrease Heart Rate, dilate pupil, constrict anal sphincter
- Peripheral Alpha 2 Adrenergic Agonists have mixed vessel effects, relaxe GI Smooth Muscle and stimulate fat cell lipolysis
- Central Alpha 2 Adrenergic Agonists vasodilate peripheral vessels
-
Beta Adrenergic Receptor
- Beta 1 Adrenergic Agonists increase myocardial contractility and Heart Rate, and increases renin release and fat cell lipolysis
- Beta 2 Adrenergic Agonists vasodilate, bronchodilate, relax Bladder wall and stimulate liver Gluconeogenesis and glycogenolysis
- Dopaminergic Receptor
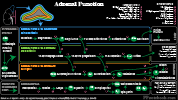
V. Medications: Sympathetic Agents
- Catecholamines: Medical and endogenous agents with Direct Sympathetic Activity
- Background: Catecholamines with Direct Sympathetic Activity
- Catecholamines, on binding alpha and beta receptors, stimulate specific Neuron second messenger release (e.g. cAMP, Inositol)
- These second messengers exert inta-Neuron effects associated with the receptor stimulated (a1, a2, b1, b2, d1-d5)
- Catecholamines are rapidly metabolized by the enzymes COMT and MAO, and have a relatively short duration of action
- Alpha Adrenergic Agonists (also have beta effects as well)
- Epinephrine
- First line agent in ACLS (VT/VFib, PEA, Symptomatic Bradycardia), Anaphylaxis, Status Asthmaticus
- Vasoconstriction (a1), Tachycardia and increased contractility (b1) and bronchodilation (b2)
- Increased Serum Glucose via glycogenolysis and Gluconeogenesis (b2) and fat breakdown (b1)
- Norepinephrine
- First line Vasopressor in fluid refractory Hypotension (esp. Septic Shock)
- Strong Vasoconstriction and increased arterial pressure (a1) and reflex Bradycardia
- Unlike Epinephrine, only small effects on contractility and NO beta effect (no bronchodilation or metabolic effects)
- Epinephrine
- Beta Adrenergic Agonists
- Isoproterenol
- Pure Beta activity, with strong vasodilation, increased Heart Rate and contractility, and bronchodilation
- Increased Serum Glucose via glycogenolysis and Gluconeogenesis (b2) and fat breakdown (b1)
- Dobutamine
- Synthetic Dopamine derivative
- Primarily B1 activity with increased cardiac contractility, and minimal increase in Heart Rate
- Only weak B2 (no bronchodilation), and minimal alpha activity (no significant change in vascular resistance)
- Isoproterenol
- Dopaminergic Agonists
- Dopamine
- Dopaminergic and B1 activity
- Has largely been replaced by Norepinephrine as a Vasopressor in adult shock (but still used in pediatric shock)
- Increases cardiac contractility, systolic Blood Pressure and to a lesser extent Heart Rate
- Dose related effects
- Dopamine
- Background: Catecholamines with Direct Sympathetic Activity
- Non-Catecholamines: Medical agents with Direct Sympathetic Activity
- Background: Non-Catecholamines with Direct Sympathetic Activity
- Similar activity to Catecholamines by acting as direct Agonists, binding alpha and beta receptors
- However, non-Catecholamines have longer duration of action, as they are not metabolized by COMT and MAO
- Alpha Adrenergic Agonists
- Phenylephrine
- Frequent use as a Push Dose Pressor in Anesthesia for Hypotension
- Strong Vasopressor with increased systolic Blood Pressure and reflex Bradycardia
- Also used as a nasal Decongestant (neosynephrine)
- Phenylephrine
- Beta 2 Adrenergic Agonists
- Bronchodilators (e.g. Albuterol, Terbutaline, Salmeterol, Pirbuterol)
- Primarily B2 activity with bronchodilation, but mild B1 activity results in Tachycardia
- Bronchodilators (e.g. Albuterol, Terbutaline, Salmeterol, Pirbuterol)
- Background: Non-Catecholamines with Direct Sympathetic Activity
- Non-Catecholamines: Illicit and non-medical agents with Indirect Sympathetic Activity
- Background: Indirect Sympathomimetics
- Unlike direct sympathetic Agonists, these agents do not bind Adrenergic Receptors
- Indirect Sympathomimetics enter presynaptic Neuron and displace Norepinephrine from their storage Vesicles
- Indirect Sympathomimetics
- Cocaine
- Blocks Monoamine Reuptake at nerve terminal
- Effects include Tachycardia, Hypertension, hyperthermia, Mydriasis, Seizures
- Amphetamines (MDMA or Ecstasy, Methamphetamine)
- Vasoconstriction, Hypertension, increased cardiac contractility, Tachycardia (or reflex decrease in Heart Rate)
- Amphetamines are used medically in Narcolepsy and Attention Deficit Disorder
- Caffeine
- Nonselective, Competitive Inhibition of Adenosine receptors
- Increases diastolic Blood Pressure and Epinephrine levels
- Cocaine
- Background: Indirect Sympathomimetics
- Non-Catecholamines: Illicit and non-medical agents with Mixed Sympathetic Activity
- Background: Mixed Sympathomimetics
- Mixed Sympathomimetics act both indirectly (Norepinephrine displacement) AND directly (Adrenergic Receptor binding)
- Mixed Sympathomimetics
- Synthetic Cathinones (Psychoactive Bath Salts)
- Inhibits Norepinephrine, Serotonin and Dopamine reuptake, resulting in increased Neurotransmitter levels
- Results in Sympathomimetic and Hallucinogenic effects (similar to Amphetamines)
- Ephedrine (Ephedra)
- Vasoconstriction, increased Blood Pressure, and cardiac contractility, no Heart Rate effect (indirect NE release)
- Bronchodilation (direct Sympathomimetic effect)
- Nicotine
- Acts at acetylcholine Nicotinic Receptors on peripheral postganglionic Sympathetic Nerves
- Stimulates Catecholamine release from Adrenal Medulla
- Sympathomimetic effects include Vasoconstriction, increased contractility and Heart Rate
- Synthetic Cathinones (Psychoactive Bath Salts)
- Background: Mixed Sympathomimetics
VI. Medications: Sympathetic Antagonists
- Central Adrenergic Agonist (presynaptic, Antagonize Sympathetic System, Antihypertensive agents)
- Peripheral Presynaptic Adrenergic Antagonist (Antihypertensive)
-
Postsynaptic Alpha Adrenergic Antagonist
- Selective Alpha-1a Antagonists: Prostate specific agents (e.g. Tamsulosin)
- Non-Selective Agents: Antihypertensives: (e.g. Terazosin, Doxazosin, Prazosin)
-
Beta Adrenergic Antagonist (Beta Blocker)
- Beta-1 Selective Adrenergic Blockade (e.g. Metoprolol, Atenolol)
- Beta-1 and Beta-2 Adrenergic Blockade (e.g. Propranolol, Nadolol, Sotalol)
- Combined Alpha-1, Beta-1 and Beta-2 Adrenergic Blockade (e.g. Labetalol, Carvedilol)
VII. References
- Olson (2020) Clinical Pharmacology, Medmasters, Miami, p. 13-33
- Goldstein (2010) Clin Auton Res 20(6):331-52 +PMID: 20623313 [PubMed]