II. Epidemiology
-
Incidence: 1 Million cases in United States annually
- Lifetime risk: 30%
- Age: Peak onset at 50-79 years old
- Gender predominance: Women account for 60% of cases
III. Pathophysiology
- Reactivation of latent virus from dorsal root Ganglion
- Initial Varicella Zoster Virus infection (Chicken Pox) recedes to cranial and dorsal root ganglia
- Occurs in 10-20% of people previously exposed to Chicken Pox
- Typically occurs when T cell mediated Immunity decreases (e.g. advancing age, Immunocompromised)
- Risk increases 20 to 100 fold over age-matched controls
- Inflammation to acute viral ID in segmental nerve
- Contagious to non-immune persons
- Avoid contact until rash heals
IV. Risk Factors
- Age over 50 years old
- Chicken Pox at age <1 year old
- Altered T cell-mediated Immunity (especially if onset in a younger patient)
- HIV Infection
- Malignancy (esp. lymphoproliferative disorders)
- Organ transplant status
- Immunosuppressant use
V. Symptoms: Prodrome
- Timing
- May be precede rash by 1-5 days
- Most common symptoms
- Fever (variably present)
- Headache
- Photophobia
- Paresthesias
- Pain within Dermatome occurs first
- Examples: itching, burning, hyperesthesia
- Malaise
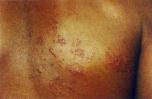
VI. Signs: Rash
- Timing
- Develops after 48-72 hours (up to 5 days before rash)
- Lesions heal within 2-4 weeks
- Distribution
- Follows 1-2 Dermatomes and uncommonly crosses the mid-line (although may occur on back)
- Lesions appear proximally first, then distally
- Most common regions
- Back (esp. T1 to L2)
- Face (esp. ophthalmic branch of Trigeminal Nerve, accounting for 15% of cases)
- Characteristics
- Associated Findings
- Tender regional Lymph Nodes
- Variants
- Zoster Sine Herpete (zoster without a rash)
- Zoster without rash is uncommon but does occur
- Gilden (2010) Curr Top Microbiol Immunol 342: 243–53 +PMID:20186614 [PubMed]
- Hutchinson's Sign (Vesicle on the tip of nose)
- Associated with Herpes Zoster Ophthalmicus
- Stain the eye for Fluorescein and observe for Dendrites
- Exercise high level of suspicion for ocular involvement
- Ramsay Hunt Syndrome (Vesicle in ear)
- Associated with Bell's Palsy
- Course may be more prolonged
- Zoster Sine Herpete (zoster without a rash)
- Images
VII. Labs: Vesicle fluid testing
- Indications
- Not routinely indicated (as Shingles is typically a clinical diagnosis)
- Recurrent lesions with suspected herpes simplex
- Suspected Zoster Sine Herpete (zoster without a rash)
- Widely disseminated rash in an immunocompomised patient
- Distinguish from other Vesiculobullous Rash (see differential diagnosis below)
- Zoster PCR (preferred)
- Test Sensitivity: 95%
- Test Specificity: 99%
- Direct immunofluorescent Antigen staining
- Test Sensitivity: 82%
- Test Specificity: 76%
-
Virus Culture
- Test Sensitivity: 20%
- Test Specificity: 99%
-
Tzanck Smear of lesion base (Multinucleated giant cells)
- Rarely performed now in United States
- References
VIII. Differential Diagnosis
- Cellulitis
- Vesicular dermatitis
- Painful serious condition (prior to dermatitis appearance)
IX. Complications
- Hospitalization in 2-3% of cases
- Postherpetic Neuralgia
-
Herpes Zoster Ophthalmicus
- Especially if Conjunctivitis or Vesicle at tip of nose
- Herpes Zoster Oticus (Ramsay Hunt Syndrome)
- Meningitis
- Encephalitis
- Granulomatous Angiitis with contralateral Hemiplegia
- Cutaneous dissemination in Lymphoma (40%)
- Diffuse involvement (including pneumonitis)
- Occurs in Immunocompromised patients
- Longterm increased cardiovascular and Cerebrovascular Disease risk
- Growing evidence for association
- Erskine (2017) PLoS One 12(7):e0181565 +PMID: 28749981 [PubMed]
X. Management: Antivirals
- Relative indications for Antivirals (maximal benefit)
- Onset within 72 hours of starting treatment
- Age 50 years and older
- More than 50 lesions
- Continued active Vesicle eruptions (even if delayed beyond the 72 hour window)
- Opthalmic or neurologic involvement (even if delayed beyond the 72 hour window)
- Includes facial involvement (due to associated risk of ocular involvement)
- Precautions
- Adjust dosing for Creatinine Clearance <50 ml/min (<60 ml/min for Famciclovir)
- Oral Antiviral Agents (oral guanosine analogues)
- Acyclovir
- Dose: 800 mg orally five times daily for 7-10 days
- Reduces healing time, pain, and rash dissemination
- Least expensive of all Antiviral options by an order of magnitude
- Valacyclovir appeared more effective in over age 50
- Valacyclovir
- Dose: 1000 mg orally three times daily for 7 days
- Equivalent efficacy to Famciclovir
- Famciclovir
- Dose: 500 mg orally three times daily for 7 days
- Lesions healed faster, more brief virus shedding
- Reduces Postherpetic Neuralgia duration by 2 months
- Reference
- Acyclovir
XI. Management: Pain Management
- See Postherpetic Neuralgia
-
Analgesics
- Schedule Analgesics around the clock (not prn)
- Mild to moderate pain
- Moderate to severe pain
- Refractory pain (agents used in Postherpetic Neuralgia)
- No evidence that these agents reduce acute Shingles pain or that they prevent Postherpetic Neuralgia
- Amitriptyline (Elavil)
- Gabapentin (Neurontin)
-
Systemic Corticosteroids
- Use is controversial and not routinely recommended
- May be associated with increased complications (e.g. Bacterial superinfection)
- May reduce acute pain, inflammation and speed up healing
- Does not reduce risk of Postherpetic Neuralgia
- References
XII. Management: Special Circumstances
- Zoster Ophthalmicus
-
Immunocompromised Patient
- Acyclovir 10 mg/kg IV every 8 hours for 10 days
XIII. Prophylaxis: Varicella Immune Globulin (VZIG) Indications
- Immunodeficient under age 15 years
- Give within 72-96 hours exposure
- Newborn of infected mother
- Exposure 5 days before delivery or 2 days after
XIV. Prevention
- Avoid contact with active Shingles or Chicken Pox
- Consider prophylaxis if exposure in high-risk groups
-
Varicella Vaccine routinely in children, teens, and adults
- May reduce risk of developing Shingles
- Part of routine Primary Series
-
Herpes Zoster Vaccine (Shingles Vaccine, Zostavax)
- Recommended in adults over age 50 years (if not contraindicated)
- Following a Shingles episode, delay Vaccination until acute Shingles has resolved prior to Vaccination (~8 weeks)
- Reduces risk of Herpes Zoster Incidence by 60% and Post-herpetic Neuralgia by 65%
XV. References
- Takhar in Majoewsky (2012) EM:Rap 12(11): 12
- Berger in Goldman (2000) Cecil Medicine, p. 2130-1
- Habif (1996) Dermatology, p. 351-9
- Gnann (2002) N Engl J Med 347:340-6 [PubMed]
- Fashner (2011) m Fam Physician 83(12): 1432-7 [PubMed]
- Saguil (2017) Am Fam Physician 96(10): 656-63 [PubMed]