III. Physiology: Clotting Factors
- Numbered Factors (typically shown with roman numerals)
- Factor 1: Fibrinogen
- Factor 2: Prothrombin
- Factor 3: Tissue Thromboplastin
- Factor 4: Calcium
- Factor 5: Proaccelerin (Ac Globulin)
- Factor 7: Proconvertin
- Factor 8: Antihemophilic Factor A (Thromboplastinogen)
- Factor 9: Antihemophilic Factor B (Christmas Factor)
- Factor 10: Stuart Factor
- Factor 11: Antihemophilic Factor C
- Factor 12: Hageman Factor
- Factor 13: Fibrin Stabilizing Factor
- Other factors
- Von Willebrand Factor (carries Factor 8)
- HMW Kininogen (Fitzgerald Factor)
- Prekallikrein (Fletcher Factor)
- Platelets
- Fibrin
- Thrombin
IV. Physiology: Clotting Factor Synthesis
-
Liver Hepatocytes (decreased synthetic function in Cirrhosis, Acute Hepatic Failure)
- Fibrinogen
- Prothrombin
- Factor 5
- Factor 7
- Factor 9
- Factor 10
- Factor 11
- Factor 12
- Protein C
- Protein S
- Antithrombin
-
Liver Sinusoidal Endothelial Cells (levels not related to hepatic synthetic function)
- Factor 8
- Von Willebrand Factor
V. Physiology: Hemostasis Mechanisms
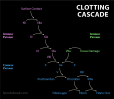
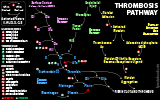
VI. Physiology: Clotting Pathways
- Initiators of the Clotting Cascade
- Intrinsic Clotting Pathway
- Initiated by Negatively charged surface of foreign material or from damaged Red Blood Cells
- Pathway is relatively slow (minutes to form blood clot)
- Factor XII to Factor XI to Factor IX and Factor VIII which trigger conversion of Factor X to Xa
- Factor Xa then proceeds into the common pathway, generating Thrombin and then Fibrin
- Extrinsic Clotting Pathway
- Initiated by disrupted cell membranes
- Damaged cells (including vascular endothelial cells) release Tissue Thromboplastin
- Pathway is relatively rapid with Blood Clotting occuring within 15 seconds
- Factor VII, Factor V and Calcium combine to trigger conversion of Factor X to Xa
- Factor Xa then proceeds into the common pathway, generating Thrombin and then Fibrin
- Intrinsic Clotting Pathway
-
Common Clotting Pathway follows above initiators
- Antagonized by Clotting Pathway Inhibition
- Prothrombin => Thrombin (catalyzed by Prothrombin activator)
- Fibrinogen => Fibrin (catalyzed by Thrombin)
- Fibrin combines with Platelets, plasma factors and Red Blood Cells to form blood clot
- Factors
- Activation
- All of these Clotting Factors (both pro-coagulant and Anticoagulant) are Vitamin K Dependent
- Vitamin K is required for carboxylation of terminal ends of coagulation Proteins
- Without carboxylation, Clotting Factors/Proteins are not activated and Clotting Cascade does not occur
- Warfarin inhibits the cyclic interconversion of Vitamin K to a reduced form
- Keeps Vitamin K and dependent factors inactive
- Procoagulant Factors (Mnemonic: "1972")
- Factor 10 (half life 36 hours)
- Factor 9 (half life 24 hours)
- Factor 7 (half life 7 hours)
- Factor 2 (half life 50 hours)
- Anticoagulant Factors
- Activation
VII. Labs
- Background: Blood collection
- Glass Blood Collection Tubes will trigger the Intrinsic Clotting Pathway
- Glass Blood Collection Tubes therefore contain Anticoagulants to prevent Blood Clotting
- Calcium (Factor 4) is a Cofactor in both the extrinsic and intrinsic pathways
- Some glass collection tubes contain Calcium binders (e.g. oxalate, citrate) to prevent clotting
- Glass Blood Collection Tubes will trigger the Intrinsic Clotting Pathway
-
Partial Thromboplastin Time (PTT)
- Measures intrinsic pathway
- Prolonged by
-
Prothrombin Time (PT)
- Measures extrinsic pathway
- Affecting both ProTime and Partial Thromboplastin Time
- Factor X
- Factor V
- Prothrombin
- Fibrinogen
-
Thrombin Time
- Measures only common pathway
VIII. Causes: Coagulation Disorder etiologies
IX. Associated Conditions
- See Bleeding Disorder
- See Thrombophilia (Hypercoagulability)
X. Resources
- Coagulation (Wikipedia)
XI. References
- Goldberg (2014) Clinical Physiology, Medmasters, Miami, p. 61-5
- Palta (2014) Indian J Anaesth 58(5): 515-23 +PMID: 25535411 [PubMed]
- Smith (2015) Crit Rev Biochem Mol Biol 50(4): 326-36 +PMID:26018600 [PubMed]