II. Differential Diagnosis: Acute Vision Loss based on pain
- Painful Vision Loss or Blurred Vision (with or without Eye Redness)
- Eye Injury
- Corneal Ulcer
- Photokeratitis
- Acute Angle-Closure Glaucoma (esp. if Intraocular Pressure >60 mmHg)
- Iritis and Uveitis (anterior chamber exudates)
- Endophthalmitis (vitreous exudates)
- Methanol toxicity
- Painless (or Minimal or variable pain) Vision Loss or Blurred Vision
- Optic Neuritis, retrobulbar Optic Neuritis or Papillitis (associated with Multiple Sclerosis)
- Eye movement may be painful
- Retinal Detachment
- Ocular tumor
- Central Retinal Artery Occlusion (pale fundus with cherry red Macula)
- Acute Maculopathy
- Pseudotumor Cerebri (or other cause of Increased Intracranial Pressure)
- Associated with Headache
- Transient Monocular Blindness (Amaurosis Fugax)
- Retinal Hemorrhage
- Optic Neuritis, retrobulbar Optic Neuritis or Papillitis (associated with Multiple Sclerosis)
III. Differential Diagnosis: Acute Unilateral Vision Loss
- Transient
- Persistent
- Acute Angle-Closure Glaucoma
- Central Retinal Artery Occlusion
- Central Retinal Vein Occlusion
- Retinal Detachment (later)
- Optic Neuritis (Multiple Sclerosis)
- Ischemic Optic Neuropathy
- Nonarteritic anterior optic Neuropathy (see Medications with Adverse Ocular Effects)
- Eye Trauma
- Tumor
- Vitreous Hemorrhage
- Occipital cortex infarction (vertebrobasilar thromboembolic event)
- Endophthalmitis
- Keratopathy
- Acute Maculopathy
- Psychogenic visual loss
IV. Differential Diagnosis: Acute Bilateral Vision Loss or Blurred Vision
- Transient
- Migraine Headache aura
- Congestive Heart Failure
- Posterior Reversible Encephalopathy Syndrome (PRES)
- Severe bilateral Carotid Artery Stenosis
- Pituitary Apoplexy (bitemporal Hemianopsia)
- Transient Ischemic Attack involving visual cortex (Hemianopsia)
- Pseudotumor Cerebri (or other cause of Increased Intracranial Pressure)
- Persistent
- Cerebrovascular Accident involving visual cortex (Hemianopsia)
- Bilateral Occipital Lobe ischemia
- Temporal Arteritis (Giant Cell Arteritis)
- Lymphoma
- Posterior ischemic Neuropathy
V. Risk Factors: Acute Vision Loss predisposing factors
- Diabetes Mellitus
- Hypertension
- Hyperlipidemia
- Hypercoagulable States
- Cardiac Arrhythmias (esp. Atrial Fibrillation, risk of embolic Retinal Artery Occlusion or CVA)
- Carotid Insufficiency
- Glaucoma
- Migraine Headaches
- Severe Myopia or Nearsightedness (Retinal Detachment)
- Recent intraocular procedures (including injections)
- Endophthalmitis
- Hypotony Maculopathy
- Choroidal effusion
VI. History
- Timing: Red flags for urgent referral
- Very recent onset of Vision Loss (hours)
- Progressive symptoms
- First episode
- Sudden onset (Hemorrhage, ischemia)
- Lesion localization
- Monocular or binocular?
- Monocular: Ocular or Optic Nerve lesion
- Binocular: Optic Chiasm and posterior back to Occipital Lobe lesion
- Focal Visual Field Deficit?
- Retina and posterior back through Optic Nerve and Occipital Lobe (post-chiasm)
- Retinal Detachment (unilateral progressive loss peripheral to central)
- Amaurosis Fugax (Temporal Arteritis with transient curtain-like closure
- Branch Retinal Artery Occlusion (BRAO)
- Cerebrovascular Accident (bilateral field deficit, Hemianopia)
- Periocular pain?
- Anterior eye or Optic Nerve lesion (requires Trigeminal Nerve sensitization)
- Acute Angle-Closure Glaucoma
- Uveitis
- Endophthalmitis
- Optic Neuritis (pain with eye movement, painless at rest)
- Disproportionate change in color Perception
- Optic Neuritis (red color desaturation)
- Monocular or binocular?
- Associated symptoms
- Nausea or Vomiting with Eye Pain
- Acute angle closure Glaucoma
- Flashes or Floaters
- Associated neurologic deficits
- Cerebrovascular Accident or other systemic cause
- Headache
- Optic Neuritis
- Migraine Headache with aura
- Pseudotumor Cerebri (Idiopathic Intracranial Hypertension)
- Temporal Arteritis (temporal Headache, Jaw Claudication, scalp tenderness)
- Nausea or Vomiting with Eye Pain
VII. Exam
-
Visual Acuity (perform with prescription lenses for distance)
- Snellen Chart
- Consider Pinhole Test for Visual Acuity in a patient who did not bring their glasses to evaluation
- Finger Counting (CF) at 1 foot and at 6 inches
- Hand Movements (HM)
- Light Perception (LP)
- No light Perception (NLP): total blindness
- Snellen Chart
-
Ciliary Flush
- Diffuse Corneal haze
- Acute angle closure Glaucoma
- Corneal opacities (especially with Fluorescein uptake)
- Diffuse Corneal haze
-
Visual Field Deficit
-
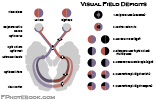
- Monocular Blindness
-
Homonymous Hemianopia (field cut affects both eyes in same region)
- Occipital lesion
-
Bitemporal Hemianopia
- Bilateral peripheral Vision Loss suggests Optic Chiasm lesion
-
-
Pupil abnormality
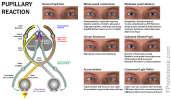
- Mid-dilated non-reactive pupil
- Relative Afferent Pupillary Defect (sluggish or absent pupil response to light, but consensual reflex)
-
Intraocular Pressure
- Acute Narrow Angle Glaucoma
-
Funduscopic Exam
-
Retinal Detachment
- Affected Retina will have the pale billowing appearance of a parachute
- In non-dilated Eye Exam, Ocular Ultrasound has better sensitivity
- Red Reflex absent or dulled
- Cherry red spot (red Macula)
-
Retinal Hemorrhage
- Central Retinal Vein Occlusion (associated with cotton wool spots)
- Other systemic causes
- Optic Disc swelling
-
Retinal Detachment
VIII. Labs
- Serum Glucose
- Inflammatory markers (CRP, ESR)
- Increased in Temporal Arteritis
-
Lactic Acid
- Increased in Methanol Poisoning
IX. Imaging
- Orbital Ultrasound
- CT Orbit
- Orbital compression (e.g. Retrobulbar Hematoma, Grave's Disease)
- CT Head with CT angio head and neck
-
MRI Brain
- Cerebrovascular Accident
- Optic Neuritis (Multiple Sclerosis)
- Neuromyelitis optica
X. Management
- Rapid assessment and management if acute CNS event is suspected
- Indications for emergent referral to ophthalmology
- Keratitis
- Endophthalmitis
- Retinal Detachment
- Retinal Hemorrhage or Vitreous Hemorrhage
- Optic Neuritis
- Occipital infarction
- Central Retinal Artery Occlusion
- Acute angle closure Glaucoma
- Ischemic Optic Neuropathy
- Conditions with specific immediate temporizing measures by emergency provider
- Ischemic Optic Neuropathy
- Central Retinal Artery Occlusion
- Acute (<4.5 hours) is treated as acute CVA with consideration for Thrombolysis (tPA, TNK)
- Acute angle closure Glaucoma
- See Acute Angle-Closure Glaucoma
- Treat with acute ocular pressure lowering (e.g. Timolol, Apraclonidine, Pilocarpine, Acetazolamide)
- Temporal Arteritis
- High dose Corticosteroids
- Temporal artery biopsy
- Methanol toxicity
- Fomepizole
- Idiopathic Intracranial Hypertension
XI. References
- Hartmann (2016) Crit Dec Emerg Med 30(6): 3-11
- Trobe (2012) Physician Guide to Eye Care, p. 31-35
- Fraser (2025) Am Fam Physician 111(1): 54-61 [PubMed]
