II. Definitions
- Aspiration Pneumonia
- Pneumonia due to food, liquid or gastric contents aspirated into the upper respiratory tract
- Aspiration Pneumonitis (chemical pneumonitis)
- Chemical aspiration of acidic gastric contents
- Degree of injury increases with gastric acidity (significant if gastric pH<2.5)
- With normal gastric acidity, Stomach contents are typically sterile
- However, not sterile in Antacid use, enteral feeding, Gastroparesis, poor Dentition and Small Bowel Obstruction
- Chemical aspiration of acidic gastric contents
III. Epidemiology
- Represents <15% of all Community Acquired Pneumonia
IV. Risk Factors
- Underlying Neurologic disease or Impairment (esp. depressed gas reflex)
- Esophageal dysfunction
- Anesthesia complication
- Microaspiration in Sleep Apnea
- Poor Dentition or severe gum disease
V. Etiology: Anaerobic Bacteria or Mixed oropharyngeal flora
- Bacteroides
- Peptostreptococcus
- Microaerophilic Streptococcus
- Fusobacterium
- Nocardia
VI. Pathophysiology
- Necrotizing infection may lead to cavitation
- Affects dependent lung lobes
VII. Symptoms
- Low grade fever
- Weight loss
- Productive cough with foul smelling Sputum
VIII. Signs
- Hypoxemia
- Tachypnea with Respiratory Alkalosis
- Wheezing
- Pulmonary Rales
- Hypotension
IX. Labs
-
Sputum Gram Stain unreliable
- Typically demonstrates mixed oral flora and many PMNs
- Sputum Culture unreliable
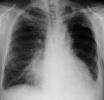
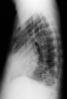
X. Imaging
- Chest XRay (often negative initially)
XI. Management: General
- Initial aspiration event results in chemical pneumonitis (not Pneumonia)
- When this is witnessed (e.g. under Anesthesia, Endotracheal Intubation), do not immediately start Antibiotics
- Await the development of Pneumonia (fever, symptoms) to institute Antibiotics
- Empiric Antibiotic prophylaxis after witnessed aspiration results in worse outcomes (e.g. Antibiotic Resistance)
- Consider early Antibiotics in Antacid use, enteral feeding, Gastroparesis and Small Bowel Obstruction
-
Antibiotics
- Typical Pneumonia organisms are more common than Anaerobes even in patients at aspiration risk
- Consider starting with typical Community Acquired Pneumonia Management
- However, start with anaerobic coverage if poor Dentition or gum disease
- Add anaerobic coverage if failure to respond to initial Antibiotics
- Antibiotic course for up to 3-4 weeks
- Extend Antibiotic course up to 2-3 months for Lung Abscess
- Typical Pneumonia organisms are more common than Anaerobes even in patients at aspiration risk
XII. Management: Oral Antibiotics
- Start with typical Community Acquired Pneumonia Management (see above)
- Consider Antibiotics listed here if failure to respond to other first-line Antibiotics (or poor Dentition or gum disease)
- First-Line
- Clindamycin 300-450 mg orally three times daily
- Moxifloxacin 400 mg once daily
- Alternative
- Amoxicillin-Clavulanate 875 orally twice daily
XIII. Management: ParenteralAntibiotics
- tart with typical Community Acquired Pneumonia Management (see above)
- First Line
- Ceftriaxone 1 g IV every 24 hours AND Metronidazole 500 mg IV every 6 hours (or 1 g IV every 12 hours) OR
- Ampicillin-Sulbactam 3 g IV every 6 hours
- Alternative
- Piperacillin-Tazobactam (Zosyn) 3.375 g IV every 6 hours OR
- Ertapenem 1 g IV every 24 hours
XIV. Prevention
- Evaluate with Swallowing Exam
- Dysphagia Diet for moderate to severe Dysphagia
XV. Prognosis: Predictors of worse outcomes
- Lower pH (<2.5)
- Larger volume aspiration (>25 ml)
- Particulate matter aspirated (e.g. food)
- Bacterial contamination (esp. Anaerobic Bacteria)
XVI. References
- (2019) Presc Lett 26(9):50
- Swadron (2019) Pulmonology 2, CCME Emergency Medicine Board Review, accessed 6/16/2019
- Gilbert (2016) Sanford Antimicrobial, accessed IOS app 12/6/2016
- Lomotan (1997) Postgrad Med 102(2):225-31 [PubMed]
- Sasaki (1997) Intern Med 36(12):851-5 [PubMed]