II. Epidemiology
- Accounts for 35-50% of Vaginitis
- HIgh recurrence rates after treatment (50% in 3 months)
III. Risk Factors
- Vaginal Douching
- Tobacco Abuse
- New or multiple sexual partners
- Unprotected intercourse
- Women Who Have Sex With Women
IV. Etiology
- Marked reduction in normally predominant lactobacillus
- Polymicrobial infection: facultative Anaerobic Bacteria
- Peptostreptococcus
- Gardnerella Vaginalis (previously classified as Haemophilus Vaginalis, Corynebacterium Vaginale)
- Facultatively anaerobic, Gram Positive, rod shaped Bacteria
- Cell wall is thin that takes up Gram Stain poorly, and may appear Gram Negative
- Bacteroides
- Mobiluncus species
- Mycoplasma hominis
- Ureaplasma
- Prevotella
V. Symptoms
- Often asymptomatic, or mild
- Musty or fishy odor to genitalia or Vaginal Discharge
- Profuse thin gray-white, non-clumping Vaginal Discharge
VI. Signs: Amsel Criteria (3 of 4 needed for diagnosis)
-
Vaginal pH > 4.5 (more alkaline than normal)
- See Vaginal pH for differential diagnosis
- Test Sensitivity: 77%
- Test Specificity: 35%
- False Positive with Cervical Mucus, Menses or semen
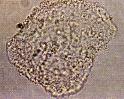
- Clue Cells present (on >20% of cells) on saline preparation
- Bacteria adhered to vaginal epithelial cells
- Test Sensitivity: 53-90%
- Test Specificity: 40-100%
- Images
- Positive whiff test (Amine Test)
- Test Sensitivity: 67%
- Test Specificity: 93%
- Volatile amines produce a fishy odor with 10% KOH
- Also present with Trichomonal Vaginitis
- Discharge characteristics
- Thin, non-clumping, gray-white, adherent discharge
- Efficacy of Amsel Criteria: At least 3 of 4 findings present
- Test Sensitivity: 70-97%
- Test Specificity: 90-94%
VII. Labs: Non-Microscopy
- High sensitivity and Specificity tests (>92% Test Sensitivity and Specificity)
- DNA Probe Test (e.g. Affirm VPIII Microbial Identification Test)
- Identifies candida, Gardnerella Vaginalis, Trichomonas
- Sialidase Activity
- Specific for Gardnerella Vaginalis
- DNA Probe Test (e.g. Affirm VPIII Microbial Identification Test)
- Older tests
- Fem Exam Card 1 (pH and amine) and 2 (Proline aminopeptidase)
- Rapid, 2 minute test with high sensitivity (91%) but low Specificity
- Trimethylamine Card for pH
- Rapid test with Low sensitivity, but high Specificity (97%)
- Fem Exam Card 1 (pH and amine) and 2 (Proline aminopeptidase)
VIII. Management
- Non-Pregnant
- Test and treat only symptomatic patients
- First-Line: Oral Metronidazole (Flagyl)
- Flagyl 500 mg orally twice daily for 7 days
- Other oral options
- Clindamycin 300 mg orally twice daily for 7 days
- Tindazole (Tindamax) 2 g orally once daily for 2 days (or 1 g orally daily for 5 days)
- Secnidazole (Solosec) 2 grams for single dose
- Sprinkle entire packet into applesauce, yogurt or pudding
- Avoid in pregnancy and Lactation
- Risk of Vulvovaginal Candidiasis
- Expensive in 2018 ($270, instead of $10 for Metronidazole)
- (2018) presc lett 25(7): 42
- Topical, intravaginal options (higher recurrence rate, does not cover Trichomoniasis)
- MetroGel (0.75%) 37.5 mg per 5g applicator intravaginally at bedtime for 5 days
- Clindamycin
- Clindamycin Cream (2%) 5g applicator intravaginally at bedtime for 7 days
- Clindamycin Ovules (Cleocin Ovules) 100 mg intravaginally at bedtime for 3 days
- Clindamycin Topicals weaken latex Condoms, diaphragms until 3 days after stopping
- Dequalinium Vaginal Tablets (not available in U.S.)
- Taken 10 mg tablet intravaginally for 7 days
- Noninferior to Metronidazole orally
- Pregnancy
- Precautions
- Bacterial Vaginosis is associated with Preterm Labor
- Treat all symptomatic Bacterial Vaginosis cases in pregnancy (but screening not indicated)
- First Trimester
- Avoid treatment if possible in first trimester
- Clindamycin (Cleocin) 300 mg PO bid for 7 days
- Clindamycin Cream 5 grams PV qhs for 7 days
- Metronidazole Gel 0.75% one applicator (5 g) PV twice daily for 5 days
- After First Trimester (prefer after 37 weeks)
- Metronidazole (Flagyl) 500 mg twice daily for 7 days
- Metronidazole (Flagyl) 250 mg three times daily for 7 days
- Clindamycin 300 mg orally twice daily for 7 days
- Precautions
- Resistant or Refractory Cases
- Metronidazole 500 mg orally twice daily for 14 days (preferred)
- Consider co-treating male-sexual partner treatment (Male Urethra may be co-infected)
- Protocol
- Metronidazole 400 mg orally twice daily for 7 days AND
- Clindamycin 2% cream applied to penis twice daily for 7 days
- Efficacy
- Decreased recurrence rates from 63 to 35% at 12 weeks
- Protocol
- Other options
- Clindamycin at above dose
- Povidone-Iodine gel OR suppository (Betadine)
- Apply vaginally bid for 14 to 28 days
- Recurrent Bacterial Vaginosis (common)
- Treat as refractory cases above (including co-treating male sexual partner)
- Combined protocol
- Metronidazole 500 mg twice daily for 7 days AND followed by
- Boric Acid gelatin cap 600 mg intravaginallyat bedtime for 21 days AND followed by
- Metronidazole vaginal gel one 5 g applicator twice weekly for 16 week
- Reichman (2009) Sex Transm Dis 36:732-4 PMID:19704395 [PubMed]
- Consider maintenance therapy
- Induction: Metronidazole gel 0.75% (Metrogel) nightly for 10 days
- Maintenance: When Wet Prep with no clue cells, pH lower
- Metronidazole gel twice weekly or (2 g oral monthly) for 3-6 months
- Treat concurrent Candida if present (e.g. Fluconazole 150 mg once monthly)
- References
IX. Complications: Sexually Transmitted Infection
- Associated with higher risk of HIV Transmission, as well as Gonorrhea, Chlamydia and Genital Herpes
X. Complications: Pregnancy
- Antibiotic treatment has not be found to reduce preterm birth risk
- Originally thought to be associated with preterm delivery (23-26 weeks)
- Originally, second trimester treatment with Clindamycin was found with better pregnancy outcomes
- Reduced preterm birth and late Miscarriage rate
- Ugwumadu (2003) Lancet 361:983-8 [PubMed]
XI. References
- (1998) MMWR Morb Mortal Wkly Rep 47:1-115 [PubMed]
- Gutman (2005) Obstet Gynecol 105(3): 551-6 [PubMed]
- Hainer (2011) Am Fam Physician 83(7): 807-15 [PubMed]
- Larimore (2000) Prim Care 27(1):35-53 [PubMed]
- Majeroni (1998) Am Fam Physician 57(6):1285-9 [PubMed]
- Miller (1997) Fam Pract 19(3):33-52 [PubMed]
- Paladine (2018) Am Fam Physician 97(5): 321-9 [PubMed]