II. Pathophysiology
- Transient disruption of a joints bone-cartilage complex
- Results in abnormal growth, injury or degeneration of developing Growth Plate
- Affects contiguous Ossification Centers in the immature skeleton
- Unknown underlying mechanism (e.g. repetitive Trauma, vascular abnormality, genetic factors)
- Precaution: Naming Alert
- Osteochondrosis is NOT the same as Osteochondritis Dissecans
III. Epidemiology
- Overall, uncommon conditions
- Gender: Boys more commonly affected
- Age: Most common between ages 10-14 years old
IV. Symptoms
- Pain or Disability at the affected joint
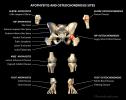
V. Types
- Back
- Scheuermann Disease (humpback deformity)
-
Elbow
- Medial Epicondyle Apophysitis
- Panner Disease (Lateral elbow capitellum degeneration)
-
Foot
- Sever Disease (Calcaneal Apophysitis)
- Frieberg Disease (second Metatarsal head)
- Kohler Bone Disease (Tarsal Navicular)
-
Knee
- Osgood-Schlatter Disease (Patellar tendon insertion at tibial tubercle Apophysitis)
- Sinding-Larsen-Johansson Disease (inferior pole Patella)
- Hip
VII. Differential Diagnosis
- Traumatic Injury
- Stress Fracture
- Avulsion Fracture
- Bony Lesions (e.g. Cancer)
- Osteomyelitis
- Inflammatory Arthropathy (multiple joints involved)
VIII. Management
- See specific conditions for management
- Conservative therapy
- Relative rest
- Ice Therapy
- NSAIDs (judicious use)
- Orthopedic or sports medicine Consultation indications
- Symptoms persists for more than 4-6 months
- Red Flags (severe pain, Trauma, inability to bear weight, night pain, systemic symptoms, cancer history)
IX. Course
- Osteochondrosis is self limited to the growth period and resolves once skeletal maturity is reached